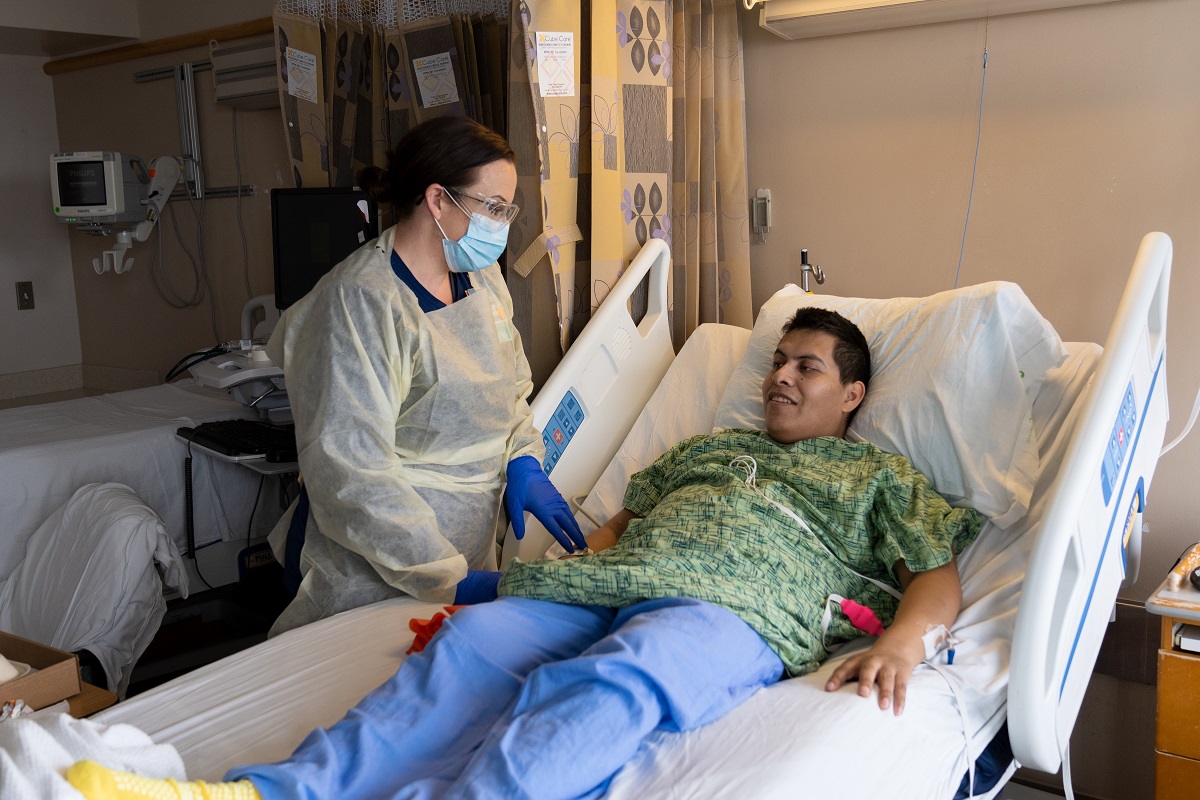
It’s 7 p.m. when Stephanie Lichtwardt, R.N., receives a call from her 10-year-old son. She’s nearing the end of a 12-hour shift in the intensive monitoring unit at UC San Diego Medical Center.
She worries. He doesn’t normally call at this time. She picks up.
“Mom, my head hurts. I’m not feeling good. Can you pick me up?”
No, Lichtwardt says to herself. There’s risk. Minimal, but it safer if she doesn’t.
If ever you could hear a heart break, it was in that moment. Lichtwardt hasn’t seen her son in person since the end of March when her unit began to care for patients severely sickened by the novel coronavirus that has shut down countries around the world, forcing millions of people to practice physical distancing—including health care workers and their families.
“He knows why he can’t see me. Still, it’s difficult to wrap my head around the idea that my job is preventing me from caring for my child and from holding him when he’s sick. I debated going to pick him up,” said Lichtwardt, pausing.
“I didn’t like my job at the end of my shift that day. I try to remember that this is temporary. A co-worker compared it to deployment. Sometimes sacrifices have to be made. My son has people who love him, who are taking care of him while I can’t. If he didn’t have a loving family to care for him, then my job wouldn’t trump being there for him.”
Lichtwardt does not believe her son would get sick if he were home with her. UC San Diego Health has supplied health care workers with the recommended personal protective equipment, such as masks, gloves and gowns, to prevent the spread of COVID-19, she said.
However, she can’t get past the idea that in the odd chance that he became infected, it might be due to her. So, her son remains under the watchful eyes of his grandparents.
He called the next morning to let her know he felt better. She did too.
“Nurses make sacrifices every day, but during this unprecedented time they are stepping up, acting courageously and being the force that leads the way in our community,” said Margarita Baggett, chief clinical officer at UC San Diego Health .
Baggett sees the impact of the pandemic on her team’s personal lives. But she also sees how they rally together, especially at work where they care for patients around the clock.
It’s particularly fitting that the World Health Organization declared 2020 as the International Year of the Nurse and the Midwife to mark the bicentenary of the birth of the founder of modern nursing, Florence Nightingale, and to recognize the critical contribution nurses make to global health.
During the COVID-19 pandemic, individuals hospitalized with COVID-19 can’t have visitors. The only people entering their rooms are health care workers bringing them medicine, food and emotional support.
While patients facing end of life are permitted visitors, that isn’t always possible for family members. In a patient’s final hours, nurses will go out of their way to set up video conferencing so that families can share those moments if they cannot be there in person.
“Patients with COVID-19 are often here with us for two to three weeks alone. Nurses become part of their extended family. One of our nurses held the hand of a patient until the final breath because family members were unable to be present,” said Baggett.
“Nursing is built upon science and the art of caring. And today, it’s come to its finest art. Every day, nurses are making history by showing up and providing exceptional clinical care for our most vulnerable.”
Nursing is much more complex than what is taught in school, said Lichtwardt. Nurses undergo training in disease process, symptom management and even psychology, but there is a lot of on-the-job training that cannot be explained in text books. Like learning to follow a gut feeling when something seems wrong, she said. That requires real-world experience.
Lichtwardt arrives for her shifts at 7 a.m. and after an update on the status of each of her patients, she begins making rounds to take vitals, administer medications and provide breakfast before trying to get a bite for herself. She repeats this at lunch and dinner time, becoming increasingly familiar with her patients as individuals with personal lives and stories.
Each patient has their own personality, so she has learned to approach each differently, from how she delivers information to how familiar she can get.
The very first person treated for COVID-19 in her unit stayed for several weeks and, because of underlying medical conditions, was very ill. Lichtwardt became very fond of him and his unswerving grace and kindness.
“He was very familiar with the hospital system and understood the importance of doing certain tests,” said Lichtwardt. “We were getting ready to take him to another room for a test when he asked me, ‘Is this really necessary?’”
“Let’s talk to the doctors,” she replied.
“I don’t want to leave this room,” said the patient. “I don’t want to get anyone sick.”
“This human being didn’t want to get lifesaving testing because of fear he might infect other people,” said Lichtwardt.
During his stay, the patient became increasingly ill and was transferred to the nearby cardiac care unit. Lichtwardt would walk over and wave through the room window so that he knew she was keeping watch.
Three times the patient was intubated, a process in which an endotracheal tube is inserted through the mouth into the airway. The tube is then connected to a ventilator to help patients mechanically breathe.
In time, the patient improved and was transferred back to Lichtwardt’s unit, where over a two-week period she helped wean him off supplemental oxygen.
Patients with COVID-19 are a prime example of what cannot be taught in a classroom. Unlike other diseases or conditions with key telltale symptoms, such as yellowing of the skin or bleeding, many patients with COVID-19 do not always show distress.
“It’s not as easy to tell when patients are in poor respiratory status, so we rely on oxygen saturation status and other skills to monitor them,” said Lichtwardt, who normally cares for people with cardiovascular disease, diabetes and kidney and liver disease.
“Sometimes, patients don’t appear to be struggling to breathe, but when we monitor them their oxygen is at 80 percent. Normal is 92 percent or above. With patients with COVID-19, we try to keep their oxygen as close to 100 percent as possible to give their lungs extra help.”
On the day Lichtwardt’s first patient with COVID-19 left the hospital, she was on duty.
“The hardest part was not being able to hug him and say goodbye. We did a fist bump in the air and laughed about it. He left the hospital walking out on his own. I wish they were all like that. His discharge … I needed to have that feeling of success. To feel that my efforts are making an impact on someone.”
Through quick learning, innovation and evidence-based care, nurses are playing a critical role during the COVID-19 pandemic, said Baggett. Collaboration among units, both those caring for patients affected by the virus and nurses caring for all other patients, is helping UC San Diego Health continue to provide the safe, compassionate and exceptional care that is expected of the region’s only academic hospital.
Nurses at UC San Diego Medical Center in Hillcrest and at Jacobs Medical Center in La Jolla bring baked goods to the teams in the emergency departments. They cook home meals for other units. They have designed 3D hairclips to keep masks from slipping and to relieve pressure on the nose and ears. They created “Caregrams,” notes of appreciation that they deliver to nurses, doctors and other health care workers throughout the hospital system to recognize each other’s efforts.
Missy Meehan, R.N., and a group of friends wrote an original melody, intended as a joyous instrumental ode to the rhythm of breathing and return to wellness, that is now played throughout both hospitals when a patient with COVID-19 is discharged.
Collaboration among nurses is not new. Lichtwardt’s colleagues are always asking how they can help each other. They give 110 percent, she said. They motivate her to push through more difficult days but then, so too do the patients.
“One patient I took care of yesterday, she’s my age and has three young kids. I want to see her recover and return home. That’s why I became a nurse,” said Lichtwardt. “If I don’t go on my shift, I don’t know who would. With the level of training I have, I’m best suited for caring for patients with COVID-19.”
Lichtwardt has been working as a nurse for 1.5 years. She began her career at UC San Diego Health and is humbled to be part of the health care heroes who are caring for people during the COVID-19 pandemic.
And while she misses her son tremendously, she cannot back away from the challenge.
“He understands. He’s more scared that I will get sick. He tells his friends that his mom is caring for patients with COVID-19. I want him to be proud. I want to be proud of myself.”
Visit the UC San Diego Health website for COVID-19 resources.
This story was originally published by University of California San Diego.